How To Treat And Care For Psoriatic Arthritis Nails
Its best to err on the side of caution and consult with your physician if youre at all worried about your nails, Dr. Garshick says. For any individual who has psoriatic arthritis and is experiencing any nail changes, it is always a good idea to talk with your doctor, since it can be important to determine if it is related to psoriasis or not, Dr. Garschick says.
Dr. Paviol suggests tracking your nail changes and how long theyve been happening in a journal. It can be helpful to make notes of other psoriatic arthritisrelated changes, such as new joint symptoms and any skin lesions. If you experience any of these nail changes and joint pain , then you may want to talk to your dermatologist or rheumatologist if you have one.
In terms of treatment, your doctor may prescribe a pharmacological medication that targets just your nail symptoms or a medication that treats your psoriatic arthritis overall. Ultimately, the treatment will depend on your specific situation.
Importantly, while some of these medications have been studied specifically for the treatment of nail psoriasis, if someone is struggling with nail psoriasis and psoriatic arthritis, it is important to consider both of these factors when selecting a treatment to be sure to select a medication that will work well for both, explains Dr. Garshick.
Related:
Causes Of Psoriatic Arthritis
Almost 1 in 3 people with psoriasis also have psoriatic arthritis.
It tends to develop 5 to 10 years after psoriasis is diagnosed, although some people may have problems with their joints before they notice any skin-related symptoms.
Like psoriasis, psoriatic arthritis is thought to happen as a result of the immune system mistakenly attacking healthy tissue.
But it’s not clear why some people with psoriasis develop psoriatic arthritis and others do not.
Characteristics Of Nail Disease
Of the 69 patients undergoing both assessments, 57 were considered by the rheumatologists to have clinically evident nail disease. The median age of onset of nail disease was 32 years , compared with 28 years for skin disease and 34 years for arthritis. Results of the detailed dermatology nail assessment, including the PNSS, are summarized in Table 1. The most frequent findings were discoloration, onycholysis and subungual hyperkeratosis. The mean PNSS was 15.5 . For fingernails, the mean PNSS was 7.4 and for toenails 8.1 . The fingernail and toenail subscores were strongly correlated . Both fingernail and toenail subscores also strongly correlated with the PNSS .
Read Also: How To Remove Contact Lenses With Nails
Your Fingernail Separates From Your Nail Bed
This condition, called onycholysis, happens when your fingernail becomes loose and separates from your nail bed, explains Dr. Garshick. Generally, the nail separates starting at the tip and travels down to where your nail meets the skin. In severe cases, people can lose their entire nail. The space created by this separation can lead to an infection, which well get to next. Furthermore, you might notice the separated part of your nail looks opaque and has a white, yellow, or green tinge, according to the Mayo Clinic. Onycholysis treatment includes topical retinoids, steroid injections, or a combination of oral medication and ultraviolet radiation therapy, according to the AAD.
What Your Nails Can Tell Your Doctor About Psa
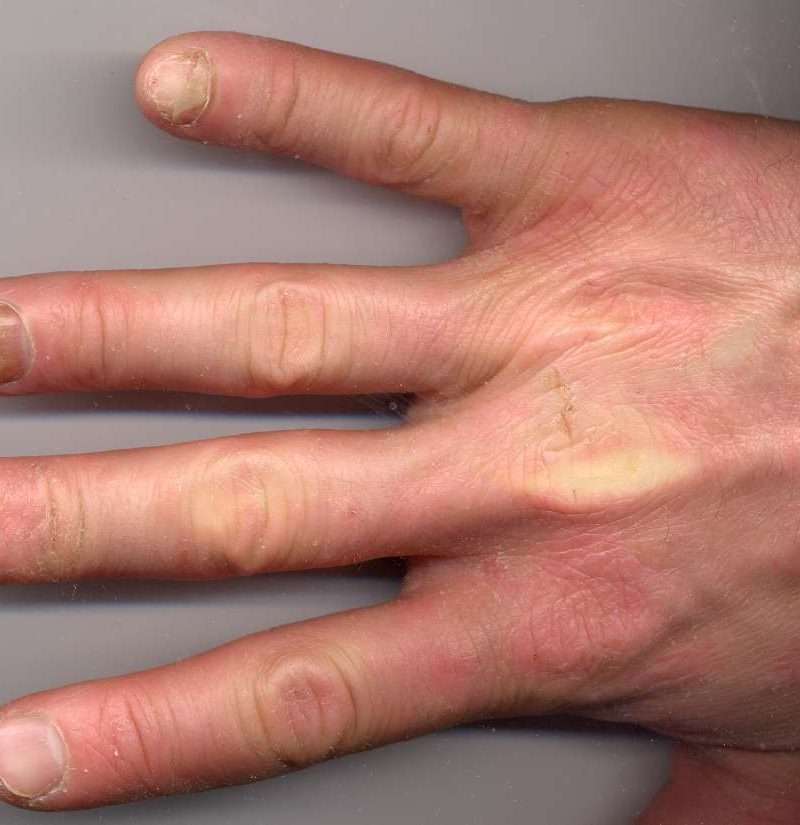
The risk of psoriatic arthritis may be evident in your fingernails and toenails.
Iâve had a complicated relationship with my nails all my life, but I pushed the symptoms aside with a shrug, thinking that my nails just didnât grow. A mani/pedi outing with the girls was always just a pedicure for me and then waiting for the others to finish getting manicures or acrylic nails put on. âWhatâs the point?â I would say to myself. âI donât have any nails to manicure, and they feel heavy enough as is.â
It wasnât until my rheumatologist was inspecting my hands that I learned there was a connection between my psoriasis, psoriatic arthritis and the condition of my nails.
The nail is composed of three main parts: the nail plate , the nail bed and the nail matrix . The part of the nail affected will determine the symptoms that show in your nail. Pits, horizontal lines, deformity, discoloration, onycholysis , brittle nails that crumble or splinter, and thickening of the nails can all be signs that nail psoriasis is present.
Apart from my pinky fingernails, every one of my fingernails is affected by nail psoriasis in some way, shape or form. My thumbnails feel heavy and have V-shaped peaks, horizontal ridges, cuticles and hangnails that crack and bleed. My ring, middle and index fingernails are brittle, have splinter hemorrhages and break in a way that reminds me of peeling away the layers of a biscuit.
Also Check: Does Dollar General Have Nail Polish
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
How Will Psoriatic Arthritis Affect Me
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body.
Psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
It will usually have some effect on your ability to get around and your quality of life, but treatment will reduce the effect it has.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissues in the body, especially if it isnt treated.
You May Like: Tips For Applying Color Street Nails
Swollen Joints Fingers And Toes
Often you’ll notice swelling in your knees, ankles, feet, and hands. Usually, a few joints are inflamed at a time. They get painful and puffy, and sometimes hot and red. When your fingers or toes are affected, they might take on a sausage shape. Psoriatic arthritis might affect pairs of joints on both sides of your body, like both of your knees, ankles, hips, and elbows.
What Are The Treatment Options For Psoriatic Arthritis
The aim of treatment for psoriatic arthritis is to control the disease and relieve symptoms. Treatment may include any combination of the following:
- Splinting.
- Surgery.
Choice of medications depends on disease severity, number of joints involved, and associated skin symptoms. During the early stages of the disease, mild inflammation may respond to nonsteroidal anti-inflammatory drugs . Cortisone injections may be used to treat ongoing inflammation in a single joint. Oral steroids, if used to treat a psoriatic arthritis flare, can temporarily worsen psoriasis. Long-term use of oral steroids should be avoided when possible due to the negative effects on the body over time.
DMARDs are used when NSAIDs fail to work and for patients with persistent and/or erosive disease. DMARDs that are effective in treating psoriatic arthritis include: methotrexate, sulfasalazine, and cyclosporine.
Biologic agents are an important consideration when disease control is not being achieved with NSAIDS or DMARDs. Biologics have been utilized for the treatment of psoriatic arthritis since 2005 and are highly effective at slowing and preventing progression of joint damage. Your healthcare provider will complete additional laboratory tests and review safety considerations before initiating a medication regimen. Gaining good control of psoriatic arthritis and psoriasis is important to avoid increased systemic risks, particularly heart disease.
Exercise
Heat and cold therapy
Splinting
Surgery
You May Like: How To Treat Nail Fungus With Vicks
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
Wear Gloves When Working With Your Hands
This includes housework, yard work, and home repairs. Any time you irritate your skin or nails, psoriasis can flare. When doing wet work like washing dishes, its best to wear a cotton glove and then place a vinyl or nitrile glove over it. According to the American Academy of Dermatology, latex gloves dont give your nails enough protection. Keeping nails dry can also make infections less likely.
Don’t Miss: Soak Dip Nails Off
Can Psoriatic Arthritis Attack Other Organs Of The Body
Apart from the skin, nails and joints, increased cardiovascular morbidity is considered part of psoriatic disease, as is the association with inflammatory bowel disease. An itchy, red eye due to conjunctivitis is more common in people with psoriatic arthritis and some people occasionally develop a painful, red eye caused by inflammation around the pupil of the eye, which is called iritis or uveitis. Anaemia may also be found but this is the result of long-term inflammation and is not a specific feature of psoriatic arthritis.
How To Hide Nail Psoriasis
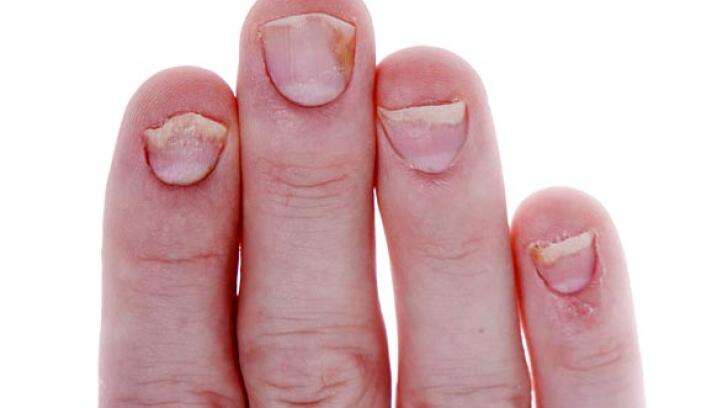
If you feel self-conscious about your nail psoriasis, there are some things you can do to make it less noticeable.
Cosmetic treatments such as nail filing, buffing, and polish can improve the appearance of your nails while they heal. Just avoid fake nails, which may increase the risk of your nail separating from its bed.
Recommended Reading: How To Get Rid Of Fingernail Fungus From Acrylic Nails
Everyday Nail Care Tips For People With Psoriatic Disease
Besides working with a rheumatologist to treat the underlying psoriatic arthritis, which is the best way to treat nail involvement, patients should follow commonsense nail care to help prevent trauma to the nail bed that could trigger more inflammation, says Dr. Shah.
Nails affected by psoriatic arthritis can break easily, and trauma can exacerbate or trigger a flare-up of symptoms. Taking steps to protect your nails is key. The American Academy of Dermatology offers a few tips that can help:
- Keep nails short. Use manicure scissors to trim nails, or file down thick toenails with an emery board. Whether or not you have psoriatic arthritis, file toenails straight across to prevent them from becoming ingrown.
- Strengthen nails. As long as your nails are intact, you may want to apply a nail hardener or even artificial nails. Just be sure youre not allergic to the chemicals and glues in these products.
- Wear gloves when doing manual labor or using soaps or chemicals. Gloves can protect nails from getting injured or irritated.
- Dont bite or pick at your nails or the skin around your nails. This can harm your nails and increase the possibility of infection.
Additional research by Becky Upham.
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Also Check: How To Remove Contact Lenses With Nails
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
What Causes Psoriatic Arthritis
The cause of psoriatic arthritis is unknown. Researchers suspect that it develops from a combination of genetic and environmental factors. They also think that immune system problems, infection, obesity, and physical trauma play a role in determining who will develop the disease. Psoriasis itself is neither infectious nor contagious.
Recent research has shown that people with psoriatic arthritis have an increased level of tumor necrosis factor in their joints and affected skin areas. These increased levels can overwhelm the immune system, making it unable to control the inflammation associated with psoriatic arthritis.
You May Like: Soaking Dip Nails Off
Which Nail Changes Are Characteristic Of Psoriatic Arthritis
Nails are involved in 80% of patients with psoriatic arthritis but in only 20% of patients with uncomplicated psoriasis, with nail involvement frequently seen at the onset when skin and joint disease begin simultaneously. The following changes in the nails support the diagnosis of psoriatic arthritis :
-
Beau lines
-
Transverse ridging
-
Cracking of the free edge of the nail
-
Uniform nail pitting: A direct correlation exists between the number of pits and their diagnostic significance
Left, typical appearance of psoriasis, with silvery scaling on a sharply marginated and reddened area of skin overlying the shin. Right, thimblelike pitting of the nail plate in a 56-year-old woman who had suffered from psoriasis for the previous 23 years. Nail pitting, transverse depressions, and subungual hyperkeratosis often occur in association with psoriatic disease of the distal interphalangeal joint. Courtesy of Ali Nawaz Khan, MBBS.
Severe, deforming arthritis of the hands and feet is frequently associated with extensive nail involvement.
Involvement of DIP joints correlates moderately well with psoriasis in adjacent nails, although this is not an invariable association. In fact, psoriatic nail changes may be a solitary finding in patients with psoriatic arthritis.
Fungal infection of the nails is the main consideration in the differential diagnosis in a patient with a seronegative polyarthritis.
How Is Nail Psoriasis Diagnosed
Nail psoriasis is usually diagnosed clinically in a patient with psoriatic arthritis and/or cutaneous psoriasis.
The severity of nail psoriasis can be estimated using the Nail Psoriasis Severity Index in which each nail is divided into quadrants and scored for clinical signs to come up with a numerical score.
Nail clippings for fungal microscopy and culture should be taken as onychomycosis may precede or complicate psoriatic nail dystrophy, and immunosuppressive medications may be used in treatment.
A proximalnail matrix biopsy is occasionally needed to confirm the diagnosis of nail psoriasis, particularly in the absence of signs of psoriasis elsewhere or where only a single nail is affected and a tumour cannot be excluded by other means. Biopsy can lead to permanent nail deformity.
Recommended Reading: How Much Does Nail School Cost
Nail Psoriasis And Psoriatic Arthritis For The Dermatologist
Rebecca Liu1, Braden M. Candela2, Joseph C English III2*
1University of Pittsburgh School of Medicine
2Department of Dermatology, University of Pittsburgh, Pittsburgh, PA
Abstract
Psoriatic arthritis may affect up to a third of patients with psoriasis. It is characterized by diverse clinical phenotypes and as such, is often underdiagnosed, leading to disease progression and poor outcomes. Nail psoriasis has been identified as a risk factor for PsA, given the anatomical connection between the extensor tendon and nail matrix. Therefore, it is important for dermatologists to screen patients exhibiting symptoms of NP for joint manifestations. On physical exam, physicians should be evaluating for concurrent skin and nail involvement, enthesitis, dactylitis, and spondyloarthropathy. Imaging modalities, including radiographs and ultrasound, may also be helpful in diagnosis of both nail and joint pathology. Physicians should refer to Rheumatology when appropriate. Numerous systemic therapies are effective at addressing both NP and PsA including DMARDs, biologics, and small molecule inhibitors. These treatments ultimately can inhibit the progression of inflammatory disease and control symptoms, thereby improving quality of life for patients.
Introduction
Figure 1: Nail psoriasis with early swelling of the distal tip of finger. Radiographic imaging demonstrated early distal PsA.
Diagnosis
Management
Figure 2: Treatment options for Nail Psoriasis and Psoriatic Arthritis
References
How Is Psoriatic Arthritis Treated
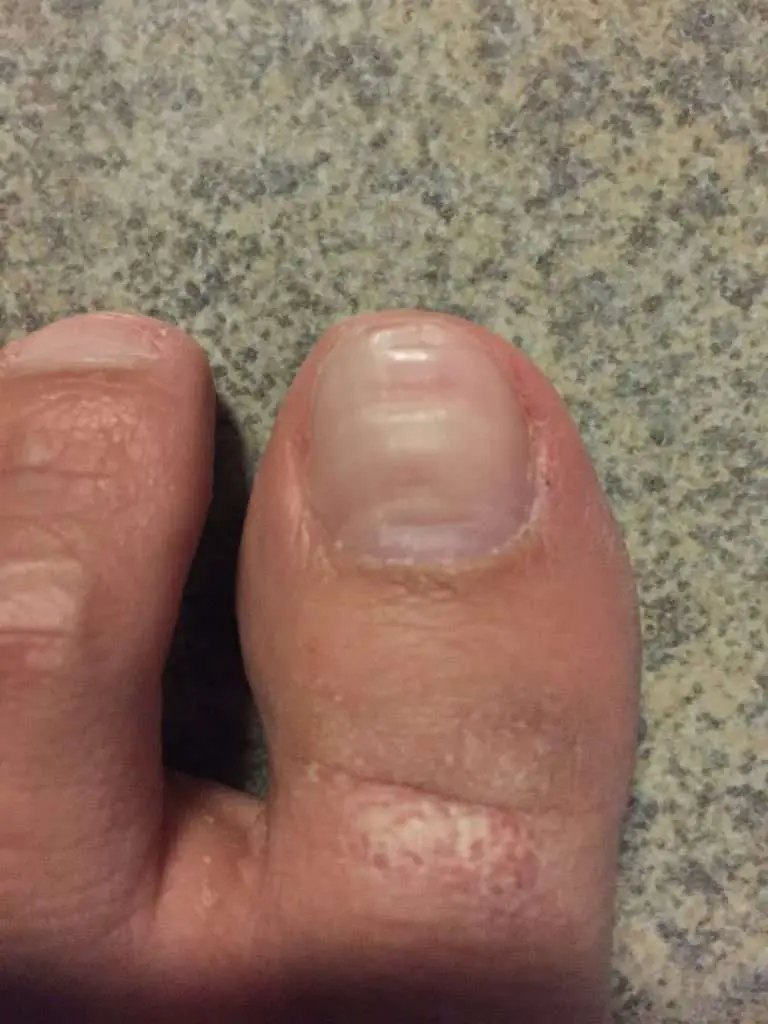
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs don’t work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
- Obesity
You May Like: Vicks Mentholatum Toenail Fungus
